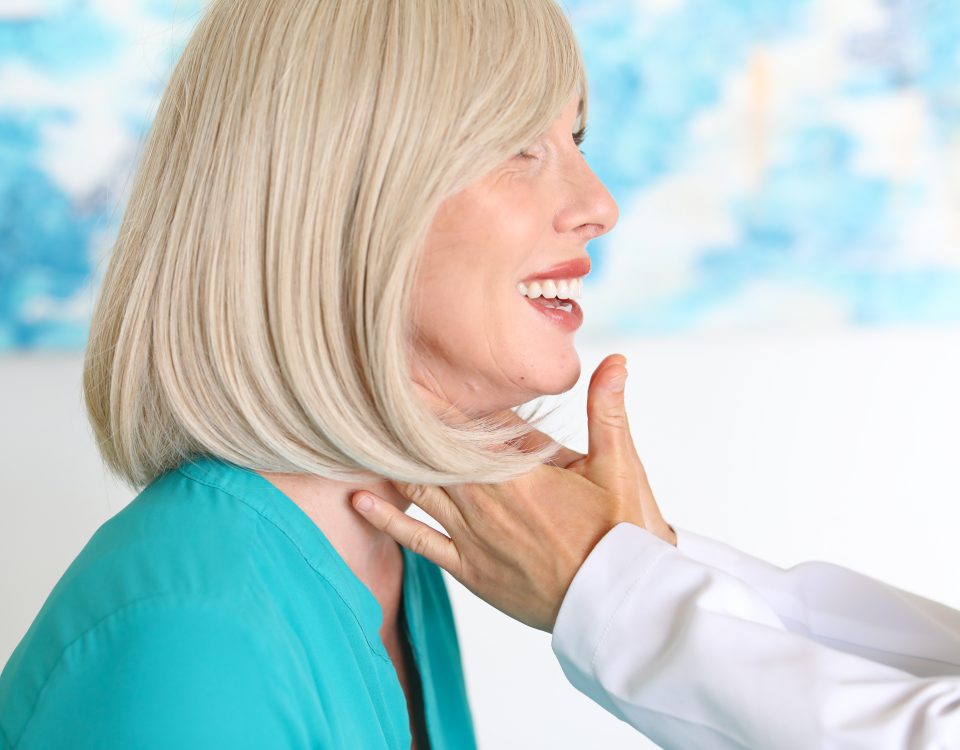
Thyroid Levels and Depression: The Latest Research
I just wanted to quickly touch on some of the research currently being done on thyroid levels and depression, which may be of use to you and your knowledge…
Antibodies and Pregnancy
One study that I found particularly fascinating had to do with high levels of thyroid peroxidase antibodies in early-to-mid pregnancy. This correlated with a higher risk for postpartum depression in these same women.1
There are not a lot of cases where these thyroid antibodies are beyond diagnostic of Hashimoto’s disease. If they are there, we have Hashimoto’s, but their absence does not rule out Hashimoto’s entirely.
Apart from this, though, there is not a lot of data that suggests that they are inherently harmful on their own.
If someone had a structurally-sound thyroid, their levels were healthy, and they were doing all the right things, but their antibodies persist, is that a danger to their health? There really is nothing that suggests that it is at this moment in time.
This data, though, runs against that. It shows that if these levels are high in the early stages of pregnancy, we may well encounter higher risks of postpartum depression thereafter. There has also been data on these same antibodies that also suggests they affect fertility.2
TSH
Thyroid stimulating hormone (TSH) is your pituitary gland telling your thyroid to work. The cycle works like this: when your thyroid makes too little hormone, your pituitary gland makes more TSH to stimulate it.
The same works when you are on thyroid hormone. If you have too little hormone, you make more TSH, and if you have too much hormone, you make less.
If you are on the high-normal side of TSH, that is a risk factor for depression that you might have not previously considered. In fact, one study looked at around 13,000 people to better understand and establish this connection.3
An equal mix of men and women, between the ages of 17 – 84, were evaluated with a symptom score based on their answers to a “Beck Depression Survey” (which results in what we call a Beck Depression Index, or BDI).
Based on their score, these participants were ultimately organized into groups. Afterward, they began correlating TSH levels to see if they could draw any conclusions. They organized them as follows: